
VOL. 10 NO. 1 THE MAGAZINE OF THE UNIVERSITY OF UTAH SUMMER 2000
 Brain
Ways
Brain
Ways
By revealing specific brain functions in real-time, advanced medical technology may lead to solutions in treating disabilities and disorders.
By Adam Olson
The other day, seven-year-old Joshua Orullian gave his grandmother a hug and said, "I love you, grandma." It almost knocked her over.
Joshua has autism. As recently as last October he struggled to put together a sentence longer than two words. Joshua was emotionally withdrawn and didn't even reach out to his own parents. "That was hard," says his mother, Julie BS'91. "Especially on his dad. He at least responded to me a little."
In 1998 Julie and Todd BS'88 MBA'89 Orullian were told about a new technology available at the University of Utah's Center for Advanced Medical Technology (CAMT). Since then, life for the Orullians has taken a new road, and the hug Joshua gave his grandmother is just one of the street markers.
Magnetic Source Imaging
CAMT was founded only a few years ago. Located in Research Park, the modest 100,000-square-foot building houses some of the most technologically advanced brain imaging equipment in the world. At the end of 1999, there were only seven other facilities across the United States that had imaging capabilities similar to CAMT's.
The technology that singles out these centers is called magnetic source imaging (MSI), which enables researchers and clinicians to receive a real-time image of how the brain functions. In other words, doctors can see which part of the brain is doing what, as it is happening. MSI melds the results of two different tests, both of which have been around for decades. Magnetic resonance imaging (MRI) reveals the appearance of the brain. Magneto encephalography (MEG) pinpoints areas of brain activity. When combined, the data offers not only new insight into how the brain functions, but also an amazing view of possible solutions to a wide variety of mental disorders.
Magnetic source imaging was made possible by improvements to magneto encephalography. In MEG, electrical current flowing within brain cells generates a surrounding neuromagnetic field, just as current flow within a power line generates a surrounding magnetic field.
MEG is most effective when many brain cells are active together. The generated magnetic field can be measured, even though the strongest magnetic signal from the brain is more than a billion times smaller than that generated by an ordinary light bulb. The brain's magnetic signature is recorded by a biomagnetometer. The University's CAMT houses two of the machines.
The emergence of MSI was dependent upon the development of more powerful biomagnetometers and the advancement of technology to the point at which MEG and MRI data could be combined correctly. It wasn't until after the mid-1980s that the conditions were right.
Still, not everyone agrees on who first created magnetic source imaging. One source says it was a group in Helsinki, Finland. Another source says it was initially developed at the Los Alamos National Research Laboratories.
Dr. William Orrison Jr., professor and chair of radiology at the University, says he was the first to combine MEG and MRI when he was part of the Los Alamos team. Orrison, who came to the University in 1997, is CAMT's medical director and one of the center's founders. He began tinkering with the MRI/MEG combination as early as 1988. While working as an associate professor of radiology and neurology at the University of New Mexico School of Medicine, Orrison earned a grant to study the correlation between MRI and MEG. He earned a second grant in 1989 to continue the study.
 Orrison's
first published report on MSI came in the July/August 1990 issue of the
American Journal of Neurology. He received a series of grants the following
year to help explore the clinical applications of MSI.
Orrison's
first published report on MSI came in the July/August 1990 issue of the
American Journal of Neurology. He received a series of grants the following
year to help explore the clinical applications of MSI.
A new approach to learning
Regardless of who put MEG and MRI together first, Orrison and the CAMT team are pioneers and visionaries in using MSI in the clinical setting.
The single most exciting thing the center could influence is "the way we teach," Orrison says, and treating learning disabilities. "We want to figure out how people learn and teach that way."
He points to three broad categories of learning styles: auditory, visual, and tactile or interactive. "In a standard classroom, that's the order of who does well," says Orrison, "because in the standard classroom, that's how we do it: we lecture. There are some visual aids if you're lucky, but there's not much hands-on doing."
Orrison believes if we can determine what kind of learner a child is, and then put the child in that kind of environment, the child will do better. However, a major obstacle to that goal is the large number of learning disorders identified in children today.
According to statistics compiled by a CAMT program called the Learning Abilities and Resource Program (LARP), one out of 10 schoolchildren in the United States has spent some time in a special education class. Speech, language, or hearing difficulties affect one child in 10. One child in three is reported to have Attention Deficit Disorder.
LARP statistics also say that special education programs serve more than five million students annually. More than 51,000 of Utah's roughly 475,000 youth are in special-education classrooms at a cost of $2,000 per child per year.
Orrison says there are also three broad categories of learning disabilities that CAMT is researching: Visual processing problems, auditory processing problems, and general information processing problems.
CAMT uses a different therapy to treat each of the disabilities: Irlen filters for visual disorders; Auditory Integration Training (AIT) for auditory disorders; and FastForWord, a computer-based training program for auditory information processing problems.
Irlen filters are colored glasses or film that are placed on a page and can counter scotopic sensitivity syndrome, a condition in which the words seem to bounce around the page.
AIT is a program that Orrison says literally reprograms the auditory cortex with specially modulated music. "A person can actually concentrate better," he says. "It's a brain function, not a hearing function." For example, a child with an auditory imbalance can easily be distracted by a fan or the hum of lights. Orrison says AIT can fix that imbalance in some cases.
FastForWord is an interactive computer program designed to improve general information processing and language skills.
MSI comes into play before and after any of the therapies is applied—first to determine which area of learning is most impaired, then to measure the effects of the therapy. "The key to the [MSI] scanning is to see who needs which therapy, and then to see if that therapy works," says Orrison. "I think it is time to redefine the approach to learning and thereby the process of teaching. It is time we modernize education.
Autism and road maps
"Autism is the second most exciting field we're working in," Orrison says. Autism afflicts more than 400,000 people in the United States and is considered to be the most severe of the pervasive developmental disorders.
"We have found through MEG evaluation that many autistic children have multifocal epilepsy. When we treat the multifocal epilepsy, their autistic symptoms may dramatically improve, which really opens the door to a whole new approach to this category of disease." In turn, CAMT researchers are pointing toward two therapies: anti-seizure medications and surgery.
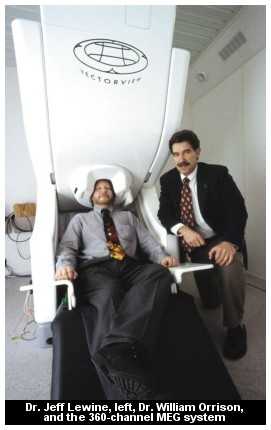
After hearing about CAMT and the work being done with MSI, the Orullians took Joshua to see CAMT Research Director Jeffrey Lewine. Various tests were performed on Joshua, including an MEG. But the Orullians were told that Joshua didn't show much seizure spiking. He was referred to a local neurologist to be put on anti-seizure medication and was monitored closely for several months.
Then in February 1999, a second MEG showed more seizure spiking. In November Joshua was sent to Omaha, Nebraska, for a series of uncommon surgeries that have been made safer thanks to MSI. In an effort to keep the epileptic foci—each a sort of seizure epicenter—from continuing to scramble normal brain activity, surgeons make superficial cuts in the brain to disrupt abnormal activity.
Before magnetic source imaging, this type of surgery was literally a stab in the dark. Surgeons had some idea of the general areas where critical brain functions such as speech and specific movements were located. But every brain is different. A cut in the wrong place could irreparably damage these essential functions.
With MSI, however, presurgical mapping of an individual's critical functions is possible to within a few millimeters. A surgeon can have a type of road map showing which areas to avoid and which areas to "disconnect."
The target: children
Despite the several beneficial uses for magnetic source imaging, the importance of this technology lies in its potential. "I predict the greatest benefits from this technology and research will come to individuals with psychiatric disorders, dementias, learning disabilities, head traumas, epilepsy, and autism," says Orrison. "That probably comprises 75 percent of the brain abnormalities in the world. That's the group we're after, as well as those who have suffered strokes or have brain tumors."
 Orrison
believes that understanding what happens inside a normal brain will throw
light on dysfunctional brains. "We haven't been able to do much for
these people previously, or even understand them. Our understanding of
what's going on with the brain in those categories is very limited."
Orrison
believes that understanding what happens inside a normal brain will throw
light on dysfunctional brains. "We haven't been able to do much for
these people previously, or even understand them. Our understanding of
what's going on with the brain in those categories is very limited."
He foresees that magnetic source imaging will lead to a dramatically improved understanding of these disorders. "That's the hope," he says. "It also provides an objective measure of the outcome of treatments, and that will lead to faster development of treatment methods as a result.
"Ninety percent of all our work is with children. This is really going to impact kids."
Not without questions
Not everyone shares Orrison's optimism. There is some controversy surrounding his work—not about MSI so much as the research that is aided by MSI, such as the learning disability and autism programs.
One doctor, speaking on condition of anonymity, voices a sentiment shared by several observers, that some of Orrison's work hasn't undergone accepted peer review in order to be substantiated and accepted. Another doctor, U of U neuroanatomist Tom Parks, says, "I have a very high opinion of Bill [Orrison] and the potential of his research." Parks adds, however, that he has concerns similar to those of other doctors. "I'm concerned about the identification of epileptic foci in kids with disorders who weren't diagnosed before."
"I predict the greatest benefits from this technology and research will come to individuals with psychiatric disorders, dementias, learning disabilities, head traumas, epilepsy, and autism."
Dr. Martin Reite, professor of psychiatry at the University of Colorado School of Medicine and director of the biomagnetic imaging laboratory, says, "MSI has a lot of potential...for looking at abnormality of function where function isn't obliterated and obvious, but impaired. I think Orrison's done some good work with that."
But Reite also has concerns about how substantiated some of Orrison's claims are by peer review, though he too won't go into specifics. "I'd have to see supporting data," he says.
In his and Orrison's field, Reite says the two ways to establish whether something is accepted by one's peers is to look at the researcher's funding—does it come from peer-reviewed funding or is it given by an outside source?—and publication results—are the researcher's papers on the subject being published by peer-reviewed publications?
The doctor speaking anonymously says Orrison's work might be better accepted if he used a more appropriate study design.
Orrison responds to this criticism by noting that his team has received three peer-reviewed autism grants totaling more than $350,000, with total grant funding of more than $2 million. His group has more than 20 peer-reviewed publications, including the lead article in Pediatrics in September 1999. He points to more than 900 peer-reviewed MEG articles available today on Medline, with more than 100 using MEG to characterize epilepsy as his group is doing.
Helping individuals
It remains to be seen if Orrison's research and research methods will produce the results he foresees and be fully accepted by the scientific community. But at least one family isn't disputing the results.
Preliminary signs indicate that Joshua Orullian's surgeries were a success. The young boy actually suffered a seizure while on the table, giving surgeons a visual guide to where the lesions occur. After three surgeries in three weeks, the Orullians were able to return home.
"It was a tough time for the family," Julie says. "But it was worth it. Any chance to let him have a better life."
And there has been a difference already. "His language has improved," she says. "Rather than having to draw him into speaking, he now responds to things around him spontaneously. He goes up to people and asks their name. Then he tells them his."
Before the medication and surgeries, Joshua spoke only one- or two-word sentences about an immediate need or want, such as, "I want drink." "That was probably his longest sentence," says Julie. "Now he goes up to people and hugs them and tells them he loves them."
Joshua's parents now feel more emotionally connected to their son. "It's like having someone in there who has found at least one little avenue to reach out from," says Julie. "He can express himself."
The Orullians know they still have rough days ahead, but they don't mind. "We're a little more optimistic about the future than before," says Julie. "He's got a long way to go, but he's definitely better off now."
—Adam Olson BS'99 writes for the Davis County Clipper and Utah Spirit magazine. His feature story on the Huntsman Cancer Institute appeared in the Spring 2000 issue of Continuum.
Copyright 2000 by The University of Utah Alumni Association